The Insurance Approval Playbook for Weight Loss Meds
Getting your insurance to cover GLP-1 medications isn't impossible—you just need to know the right moves and what documentation actually works.
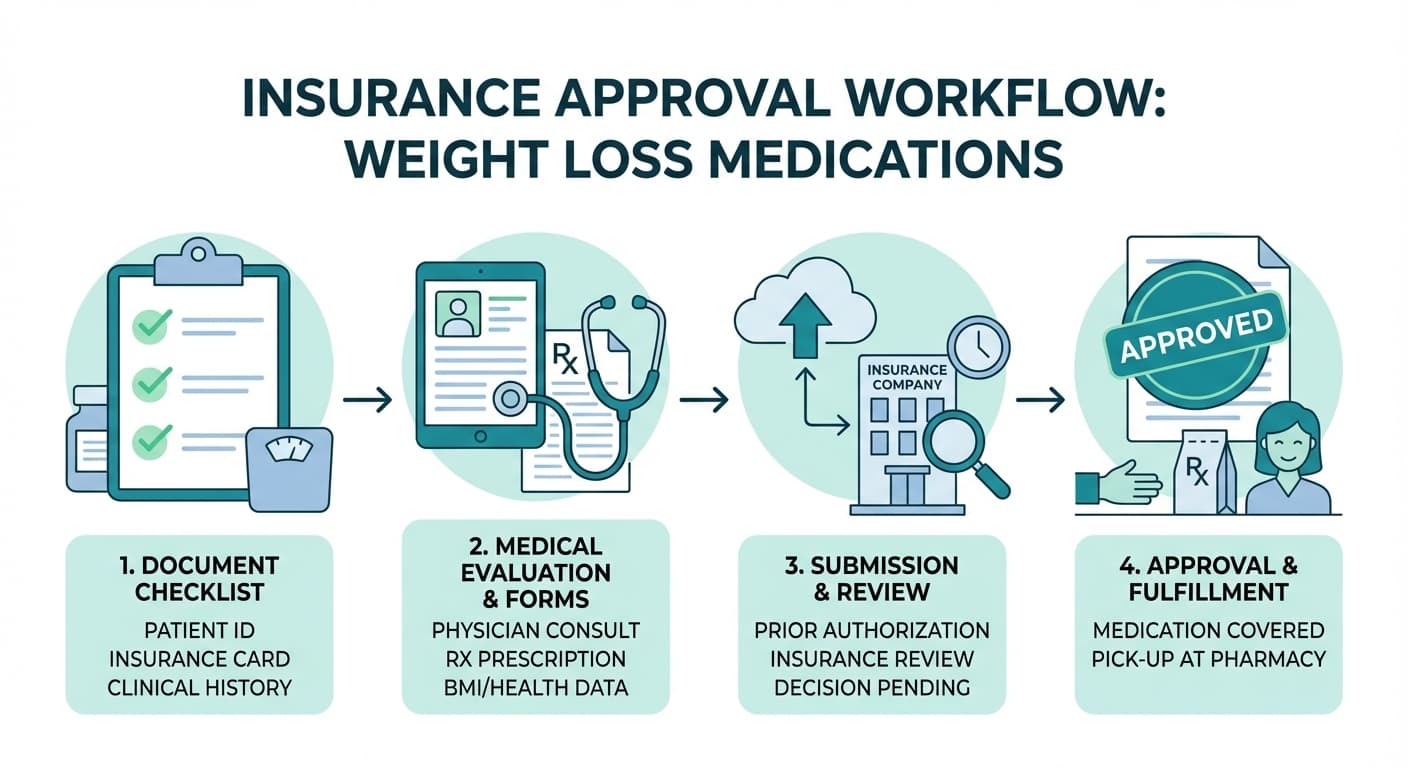
The Documentation That Actually Gets Approvals
Here's what I wish someone had told me before I started this whole insurance dance: your doctor saying "this patient needs Wegovy" isn't enough. Insurance companies want a paper trail that tells a story.
Start with your BMI documentation over time. Most insurers require a BMI of 30 or higher, or 27+ with comorbidities like diabetes or high blood pressure. But here's the thing—they don't just want today's number. They want to see that this has been consistent over at least 6 months.
Your medical records should show documented weight loss attempts. This means formal programs, not just "I tried keto once." Think medically supervised diets, Weight Watchers with weigh-in records, or consultations with registered dietitians. The more official documentation you have, the stronger your case becomes.
The Prior Authorization Strategy That Works
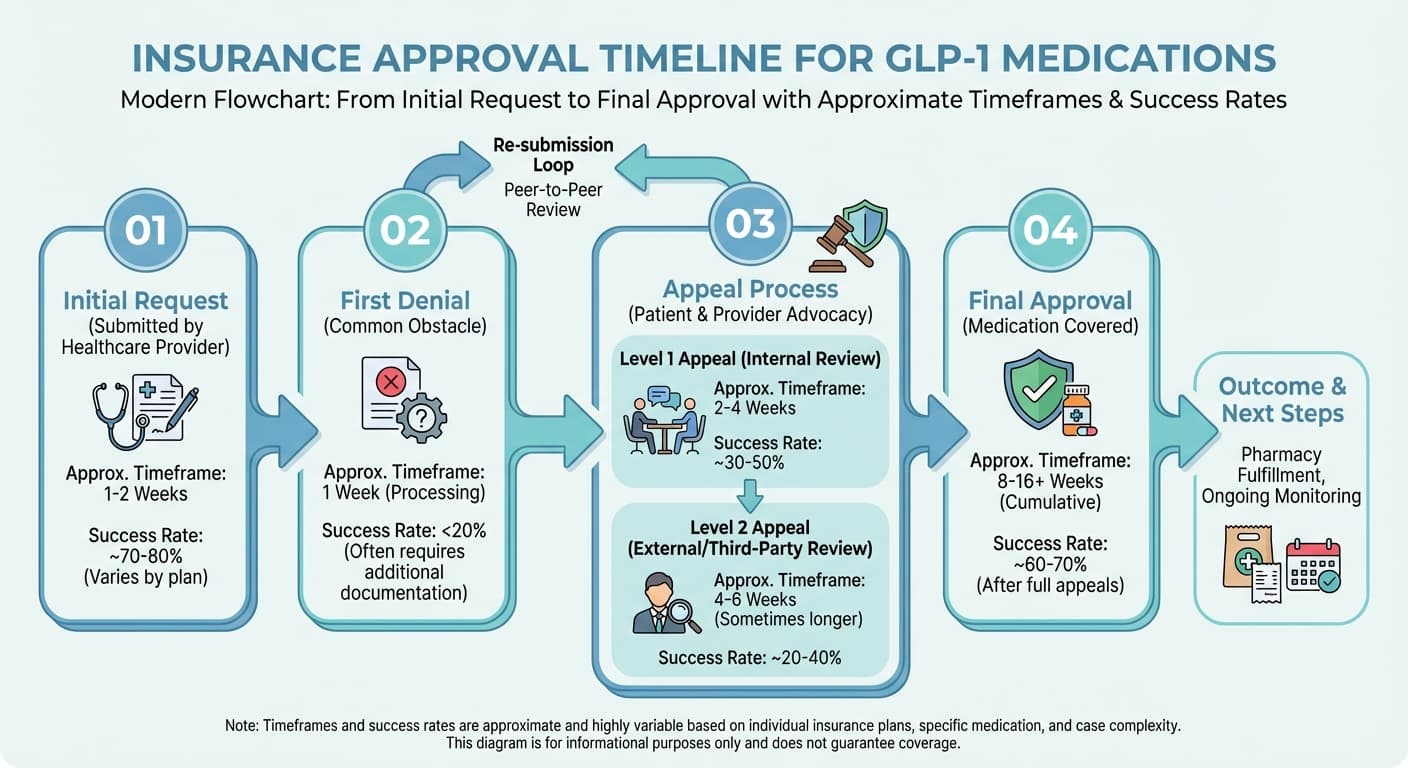
Real talk: most GLP-1 medication requests get denied on the first try. Insurance companies count on you giving up after that initial "no." Don't.
When your doctor submits the prior authorization, make sure they include:
- Complete medical history showing obesity as a chronic condition
- Documentation of weight-related health issues (sleep apnea, joint problems, high blood pressure)
- Records of previous weight loss attempts with dates and outcomes
- Clear medical necessity statement explaining why this specific medication is needed
If you get denied, ask for the specific denial reason in writing. Sometimes it's as simple as missing lab work or needing additional documentation from a specialist.
Working the System: Appeals That Win
The appeal process is where persistence pays off. Most people don't realize that denial rates drop significantly on appeals—insurance companies know that only the serious cases make it this far.
For your first appeal, have your doctor write a detailed letter explaining:
- Why other weight loss methods haven't worked for your specific situation
- The health risks you face without treatment
- How this medication fits into your overall treatment plan
Second appeals often require peer-to-peer reviews where your doctor talks directly to the insurance company's medical director. This is actually good news—doctor-to-doctor conversations tend to be more productive than paperwork battles.
The Comorbidity Advantage
Insurance companies are much more likely to approve coverage when obesity isn't your only health concern. Type 2 diabetes is the golden ticket—most insurers readily cover semaglutide and tirzepatide for diabetes management, even when weight loss is your primary goal.
Other conditions that strengthen your case:
- Sleep apnea (especially if you use a CPAP machine)
- High blood pressure requiring medication
- High cholesterol or triglycerides
- Non-alcoholic fatty liver disease
- Polycystic ovary syndrome (PCOS)
- Prediabetes with documented progression risk
If you have any of these conditions, make sure they're prominently featured in your prior authorization request.
Plan Shopping: Not All Insurance Is Created Equal
If you're shopping for insurance during open enrollment, coverage for weight loss medications should factor into your decision. Some plans explicitly exclude obesity treatments, while others have surprisingly good coverage.
Call the insurance company directly and ask about coverage for "anti-obesity medications" or "weight management treatments." Don't just ask about specific drug names—formularies change, but coverage policies tend to be more stable.
Employer-sponsored plans often have better coverage than individual marketplace plans. If you have options, compare the total cost including premiums, deductibles, and medication copays.
The Formulary Dance
Insurance formularies—the lists of covered medications—change constantly. Your plan might cover Ozempic but not Wegovy, or Mounjaro but not Zepbound, even though these are essentially the same medications with different FDA approvals.
Sometimes the path of least resistance is asking your doctor to prescribe whichever GLP-1 medication your insurance covers, rather than fighting for a specific brand. When you're looking at different options, the clinical outcomes are remarkably similar across the class.
Employer Health Benefits: The Hidden Opportunity
Many people don't realize that employer health benefits are negotiable—not for you individually, but for your company as a whole. If your employer's plan doesn't cover weight loss medications, it might be worth bringing this up during benefits review periods.
Employers are increasingly interested in covering treatments that reduce long-term healthcare costs. Weight loss medications can prevent or improve diabetes, reduce cardiovascular events, and decrease the need for joint surgeries—all of which save money in the long run.
State-by-State Variations
Some states have laws requiring insurance coverage for obesity treatments. These vary widely, but they can override federal guidelines in your favor.
States with stronger obesity treatment mandates include:
- California
- Connecticut
- Maryland
- New Jersey
If you live in one of these states and your insurance denies coverage, mention the state mandate in your appeal.
When Insurance Still Says No
Even with perfect documentation and multiple appeals, some insurance plans simply won't budge. At that point, you're looking at alternative strategies.
Manufacturer savings programs can bring brand-name medications down to $25-$50 per month, but these usually exclude government insurance like Medicare or Medicaid. Commercial insurance patients often qualify.
Some people find that switching to a diabetes indication works when weight loss doesn't. If you have prediabetes or early type 2 diabetes, your doctor might prescribe the same medication for blood sugar control rather than weight management.
The Long Game
Insurance coverage for GLP-1 medications is expanding rapidly as the evidence for cardiovascular and other health benefits grows stronger. What gets denied today might be standard coverage next year.
If you can't get coverage now, document everything. Keep records of your weight, health conditions, and treatment attempts. This creates a stronger case for future authorization requests and appeals.
The key is persistence without desperation. Insurance companies are businesses making calculated decisions based on documentation and policies. Give them the paperwork trail they need, follow the process methodically, and don't take the first "no" as final.